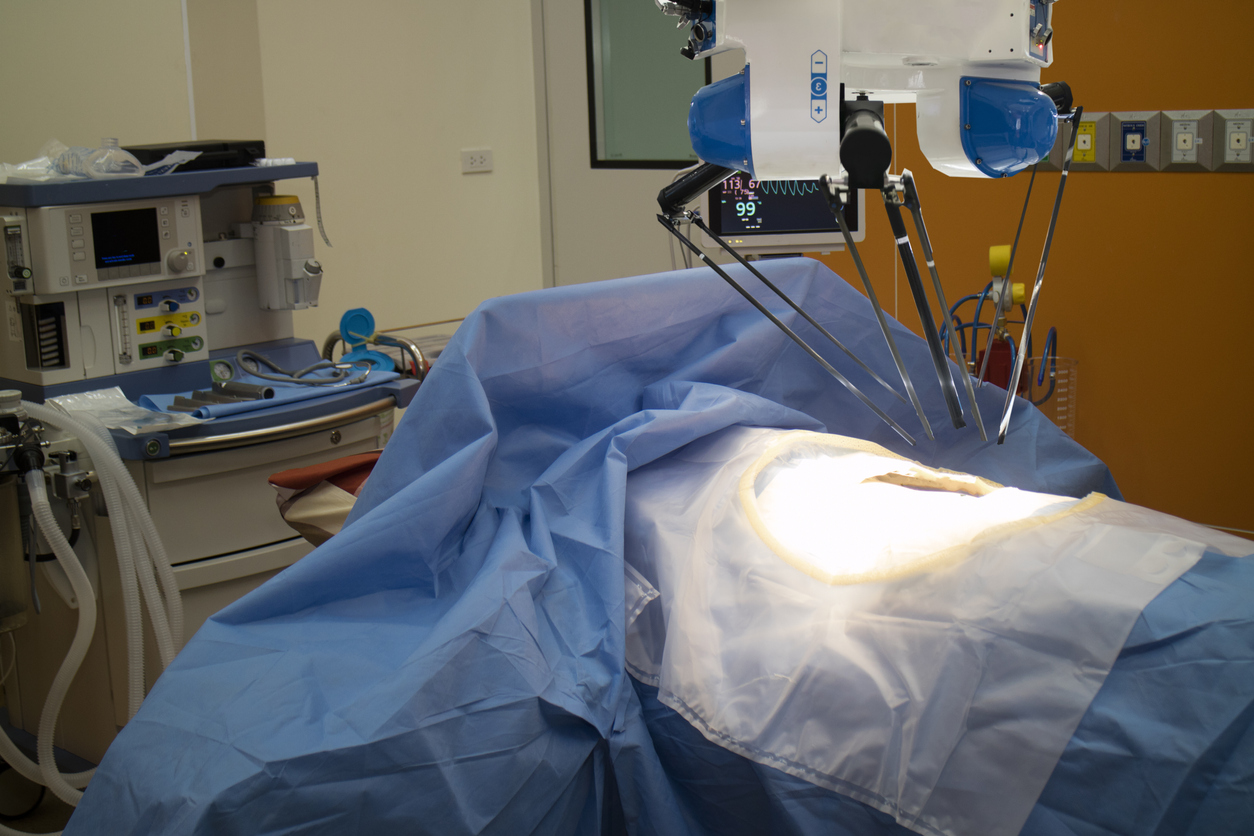
Recent developments allow surgeons to do operations remotely by guiding mechanical arms, rather than needing to be next to the patient. This is called robot-assisted surgery and the Cochrane Review of its use in gynaecological surgery was updated in October 2018. Theresa Lawrie from the Cochrane Gynaecology, Neuro-oncology and Orphan Cancer Group based in Bath in the UK, tells us the latest.
Robot-assisted surgery is used in several countries for gynaecological surgery, particularly for removing the uterus, known as a hysterectomy, and also for other procedures including removal of uterine fibroids, restoring fertility, and repairing vaginal vault prolapse. This last procedure is known as sacrocolopexy. The approach has also been used for the treatment of women with endometrial and cervical cancers.
However, robot-assisted surgery is controversial because of the significant commercial interests involved and because the potential benefits and harms over standard surgical approaches have not been clearly established. Unfortunately, despite our updating of the previous version of this review, which was published in 2014, we’re still not able to fully resolve the uncertainties. Much of the evidence remains low quality, and we cannot be sure whether there is a difference between robot-assisted and conventional laparoscopic, or keyhole, surgery in overall complication rates and other outcomes for the patients.
We now include 12 randomised trials, involving just over a thousand women. Eight studies compared robot-assisted surgery with conventional surgical approaches for hysterectomy, three looked at sacrocolpopexy and the last examined surgical treatment for endometriosis. Among studies of women undergoing hysterectomy, two involved women with endometrial cancer while the others involved women with benign conditions.

For hysterectomies, when robot-assisted and conventional laparascopic surgery were compared, we could not be sure whether there was a difference in complication rates during or after the operation, for either benign disease or cancer. Two studies did show that robot-assisted operations took about 40 minutes longer than conventional approaches, but hospital stays were slightly shorter. However, the evidence for these findings was of very low certainty, partly because of the high risk of bias in the trials. One study compared robot-assisted surgery with open abdominal surgery for hysterectomy; but it was too small, with just 20 women, to be able to detect any possible differences between the two techniques.
For sacrocolpopexy, limited data from three studies suggest that, overall, there may be little or no difference in the rate of complications during the operation between robot-assisted and conventional surgery. However, low-certainty evidence from a single study suggests that post-operative complications might be higher with robot-assisted techniques. With regard to operating time, robot-assisted surgery for sacrocolpopexy might be associated with longer operations than conventional surgery, but the duration of hospital stay was similar for the two procedures.
Finally, the one study of robot-assisted versus conventional surgery for endometriosis, was, once again, too small to show potential differences between these surgical approaches.
In conclusion, low-certainty evidence for hysterectomy and sacrocolpopexy operations suggests that complication rates for robot-assisted surgery might be similar to those for conventional laparoscopic surgery. Things are more uncertain for gynaecological cancer, where we found no comparative evidence on cancer recurrence or survival after the surgery. As robot-assisted surgery depends on the skill and experience of the surgeon and is expensive, evaluating its effectiveness and safety continues to present a challenge; but this needs to be met if we are to have reliable evidence on its potential benefits and harms.

