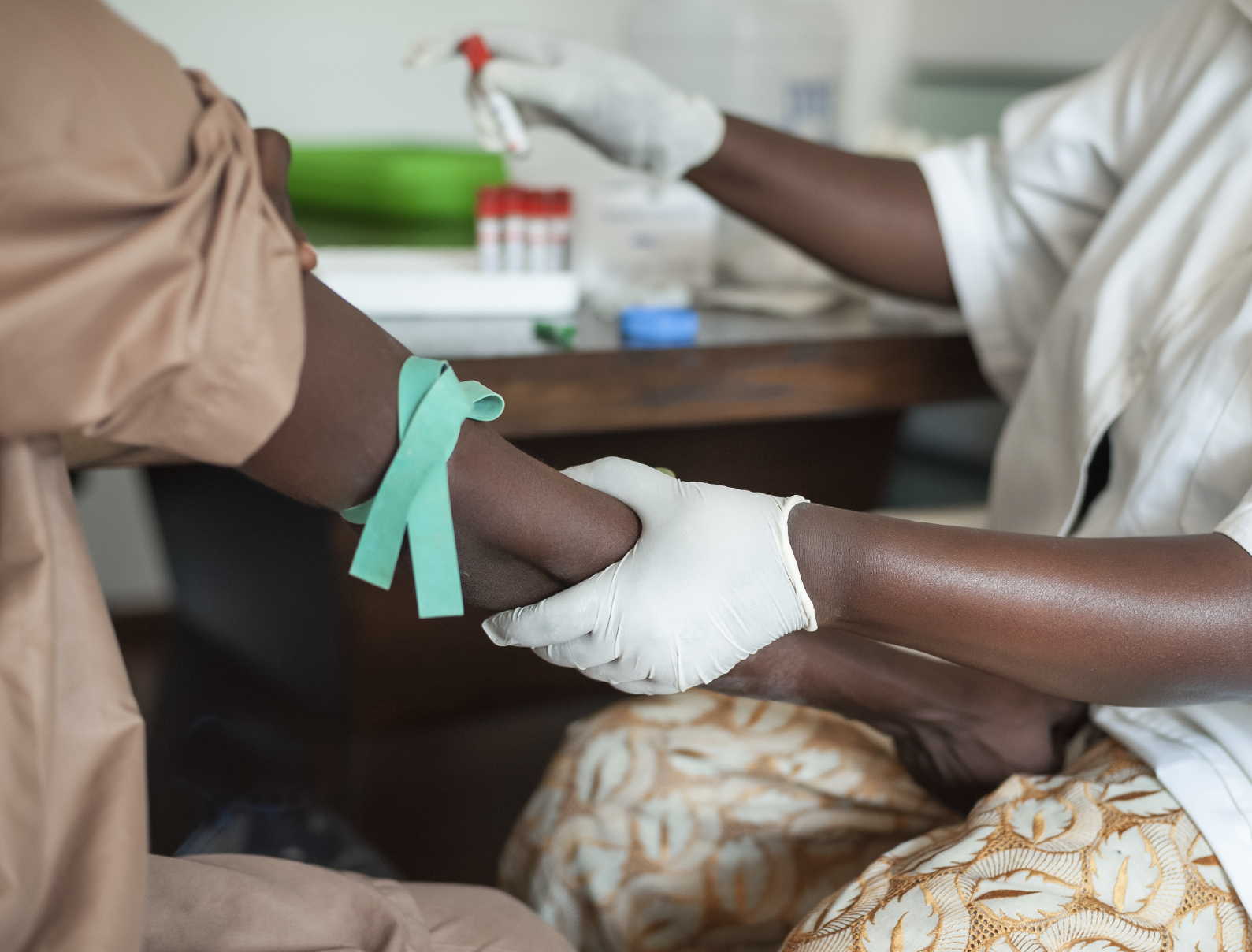
The Authors' story
The Cochrane authors of ‘Health system and community level interventions for improving antenatal care coverage and health outcomes’ share the background of the review, the evidence they found, and their recommendations.
Background to the review
Pregnant women in low- and middle-income countries (LMICs) suffer disproportionately from maternal deaths due to complications of pregnancy and childbirth. Neonatal death rates are also high in these settings. Improving access to antenatal care during pregnancy may improve outcomes for women and infants because antenatal care is positively associated with pregnant women delivering in health facilities and with more babies born of normal birthweight.
The World Health Organization recommends that all pregnant women receive at least four antenatal care visits. Ideally, pregnant women would have access to evenly spaced visits from the first trimester, with components of care including infection screening, nutrition advice, education on pregnancy and birth warning signs, and care of the new born. Many pregnant women miss out on this level of care.
Our Cochrane Review brings together evidence from randomized clinical trials of interventions to improve antenatal care coverage (ANC), to better understand efforts that improve coverage, and the consequent impact on pregnant women and their babies. We looked at trial evidence for two primary outcomes: pregnant women receiving at least four ANC visits, and maternal deaths due to complications of pregnancy or childbirth. Other important measures included women having one or more ANC visits, women delivering in health facilities, perinatal mortality, low birthweight, and women receiving prophylactic intermittent treatment for malaria.
Trials in our review tested different strategies for improving antenatal care coverage. Some interventions targeted health systems, including improved facilities and equipment, education for health providers, improved systems of referrals, use of lay health workers, or additional clinic or home visits for pregnant women. Other interventions targeted pregnant women directly, such as health, nutrition, and pregnancy education; women’s groups to improve social and community support networks; and media campaigns and financial incentives to improve uptake of antenatal care services.
What evidence did we find?
Our review included 34 trials with 400,000 women. Most trials were set in LMICs. Because most trials were conducted according to current standards, we were confident to trust the reported results. The quality rating below associated with each outcome (high, moderate, or low evidence) shows our level of confidence that the result is robust and meaningful to future research.
Trials comparing one intervention with no intervention
Single interventions to improve uptake of antenatal care marginally improved the numbers of women who attended at least four ANC visits (10 trials; 45,022 women; high quality evidence). There was inconclusive evidence as to whether a single intervention could improve rates of maternal death (10 trials; 114,930 women; low quality evidence) or low birthweight (5 trials; 27,154 infants; high quality evidence). There was no evidence that single interventions reduced rates of baby deaths (15 trials; 189,074 infants; moderate quality evidence). However, single interventions led to modest improvements in the number of women who had at least one ANC visit (6 trials; 19,281 women; moderate quality evidence) and who delivered in a health facility (10 trials; 74,299 women; high quality evidence). Trials of single interventions did not report the number of women who received intermittent preventive treatment for malaria.
Trials comparing two or more interventions with no intervention
There was inconclusive evidence that combined interventions improved the numbers of pregnant women who had four or more ANC visits (6 trials, 7,840 women; low quality evidence). There was no evidence that combined interventions were able to reduce maternal deaths, but only three trials reported this outcome (13,756 women; moderate quality). There was also no clear evidence that multiple interventions increased the number of women who delivered in a health facility (5 trials; 12,314 women; moderate quality). However, many more women who received combined interventions had one or more ANC visits (5 trials; 12,426 women; moderate quality). Combined interventions also led to fewer baby deaths (5 trials; 39,130 infants; moderate quality) and fewer low birthweight babies (2 trials; 2,084 infants; moderate quality). No trial reported the number of women who received intermittent preventive treatment for malaria.
What is the bottom line? Improved antenatal care coverage impacts neonatal deaths and low birth weight.
Efforts to improve antenatal care coverage work, with more women receiving antenatal care. Improved coverage of antenatal care also impacts the health of newborn infants.
Single interventions improve the proportion of women attending at least one ANC visit and women attending four or more visits; more women receiving the single intervention were also more likely to give birth in a health facility. Combined interventions improved the proportion of pregnant women receiving at least one ANC visit, and reduced both baby deaths and the number of babies born with low birthweight. More good quality trials of combined interventions are needed.
Read the full review.
Visit the Cochrane Pregnancy and Childbirth website.

